The Gallbladder Page
By Daniel Selby
Updated February 2, 2025 -
New Information at bottom!
Hello,
This page was written for those who are experiencing problems with their gallbladders and have questions about what some of the options are to going about getting rid of the problem. I have had severe gallstone problems and have passed stones on at least three different occasions before I took action. A lot of times gallbladder problems start as stomach problems.
I am not a medical doctor, I am simply a person who had a problem with gallstones and looked at all the options for treatment before choosing one that worked for me. Over the last month I have learned a lot about an organ I had not thought much about before (except when it gave me pain). I do not mean to scare anyone, but gallbladder disease is not something to be taken lightly. This is what I have found and what has worked for me. I hope it helps you decide what to do too, whatever it is that you decide. For a picture of the gallbladder/biliary system please see the bottom of the page.
First Some History:
What is a Gallbladder?
The gallbladder is a small (4 inches in length) pear shaped organ located on the underside of the liver on the right side of the abdomen. The function of the gallbladder is to store and concentrate bile that is produced in the liver before the bile is secreted into the intestines through the bile duct. Bile secreted into the intestines helps the body digest fats.
What are gallstones?
Bile is composed of three major components: cholesterol, bile salts, and bilirubin. When the gallbladder is not functioning correctly, the components of the bile can get out of balance leading to the formation of solid crystals, which over time, become gallstones. The majority of stones (80%) are composed of cholesterol; the remainder are pigmented stones consisting of bilirubin. Stones can be large or small, single or multiple. I had so many they could not count them on my ultrasound! These factors do not necessarily predict the frequency of symptoms or the severity of the disease. In many cases gallbladder symptoms are caused by a dysfunctional gallbladder that is forming stones rather than the stones themselves. The exception to this is when stones block off the cystic or common bile duct.
Symptoms of Gallbladder disease:
Asymptomatic cholelithiasis - The great majority of patients with gallstones (40%) have no symptoms at all. Stones in these patients are found incidentally during medical tests for other conditions or at autopsy.
Biliary Colic - For patients who do have symptoms, gallbladder symptoms can be variable. Classic gallbladder attacks consist of upper right quadrant abdominal pain, which is pain just under the rib cage on the right side. The pain often radiates around the abdomen to the back and is associated with nausea and oftentimes vomiting. The pain is severe and lasts from 30 minutes to several hours. Other symptoms that can occur during biliary colic include: severe sweating, chills, diarrhea and dizziness. Often this is followed by less intense soreness in the area that lasts for a day or so. Attacks are often instigated by a fatty meal. Gallbladder disease can also cause chronic nausea.
Cholecystitis - A more serious form of gallbladder disease, cholecystitis is an infection or inflammation of the gallbladder often caused by obstruction of the cystic duct. The symptoms are similar to biliary colic but more prolonged. Patients can also have fever, chills and an elevated white blood cell count.
Choledocholithiasis (common bile duct stones) - Stones can move out of the gallbladder and into the common bile duct. These stones often pass into the intestines along with the bile and then out with a bowel movement without incident. But sometimes they can cause obstructions in the bile duct leading to jaundice (the yellowing of skin and eyes) and life threatening infections of the bile ducts.
Biliary pancreatitis - When stones pass down the common bile duct and by the pancreatic duct they may become lodged. This can lead to the pancreas becoming irritated leading to potentially serious conditions, due to the pancreas not being able to secrete digestive enzymes out and into the intestine via the pancreatic duct which meets the bile duct at the hepatopancreatic ampulla. Symptoms of this condition usually consist of mid-abdominal pain radiating to the back with nausea and vomiting. If the stone does not make it's way into the intestine or is not treated the pancreas can become infected leading to the organ digesting itself and even to pancreatic tumors or cancer.
Other possible problems include: Empyemia of the gallbladder, this is a rare complication where the organ becomes infected and greatly distended with pus and can rupture. In very rare cases, rupture of the bile duct occurs also, followed by fatal peritonitis.
How are gallbladder problems diagnosed?
These are some of the basic tests used to evaluate the above conditions. I had all of these done. They include:
Lab Tests: to check for jaundice and signs of liver inflammation.
Blood Amylase level: to check for pancreatic inflammation.
Ultrasound: Uses sound waves to image the intra-abdominal organs including the gallbladder. On my ultrasound results my gallbladder was found to have a thickening of the walls, suggesting many previous attacks, stopping just short of rupture. I did not have pus or infection- (thankfully!) just pressure from a blocked stone.
CT Scan: Computer constructed x-ray images of the abdominal organs.
Heida Scan: Uses a low level radioactive tracer that is taken up by the gallbladder to measure gallbladder
function. It shows how well the gallbladder empties when triggered.
MRCP: A type of MRI scan that visualizes the common bile duct to check for bile duct obstruction.
ERCP: A test where a scope is passed via the mouth into the common bile duct allowing dye to be injected into the common bile duct. X-ray pictures are then taken. This test gives the most accurate assessment of the
common bile duct. It also is sometimes required to extract stones from the common bile duct.
What are some of the treatments for Gallstones?
The Gallbladder Flush
I have never done this, but if you ask me these flushes do not and cannot work. For this type of "treatment" you drink a mixture of virgin olive oil and lemon juice, occasionally with some Epsom salts added. This mixture is supposed to somehow get from your intestines up into the common bile duct and then up even further into the gallbladder to wash gallstones out. This is not possible for the very reason that at the end of the common bile duct sits the major duodenal papilla (aka hepatopancreatic ampulla) which is where bile and pancreatic digestive enzymes enter into your intestines from your gallbladder and pancreas when signaled by hormones. This major duodenal papilla is a sphincter muscle that is very much like your anal sphincter and it remains closed until it is signaled to open and release bile/pancreatic digestive enzymes when your gallbladder contracts and forces them into your intestines after a meal. The claim is that the lemon juice signals the opening of the sphincter allowing the oil in to lubricate the bile ducts and wash out the stones. If this did work, one of my questions is: What prevents the stones from washing up into the liver on that tidal wave of oil? Those who claim to get "gallstones" out after one of these treatments need to look closely at the so-called "stones." They are the product (result) of your stomach and intestines digesting (processing) the oil and lemon juice and they lack any of the chemical composites that real gallstones have. Real gallstones are very hard, not soft and soapy, as these washed out "stones" tend to be. This treatment may help clean out your intestines to a certain degree, but can in no way make it up into your gallbladder and wash out gallstones. Think of this: Whenever you drink lemonade, which has a lot more lemon juice than the little amount added to one of these "flushes," does that sphincter open then, letting the juice get in? I don’t think so. This cannot work. The body prevents anything from entering the major duodenal papilla. It is a "One Way Street" or an "Exit Only" if you will.
Dissolving Gallstones
Do not believe anyone online (or anywhere else) claiming that you can dissolve gallstones "naturally." Without a drug called Ursodiol or Chenodiol that simply is not possible. Ursodiol and Chenodiol are used in the medical field to dissolve stones, but there are important limitations to the use of Ursodiol (and Chenodiol):
It is only effective for cholesterol gallstones NOT pigment gallstones.
It works only for small gallstones, less than 1-1.5 cm in diameter.
It also takes 1-2 years for the gallstones to dissolve, and many of the gallstones form again following stopping of treatment.
Those claiming to have an e-book or potion to sell you that "really works" are only after your money. They do not care about your health- only your wallet. I wrote to a man selling an e-book on line and asked about it. He told me to look elsewhere for help. Please, don’t be fooled by these people- they are phonies.
Contact Solvent Dissolution
For this other medical stone dissolving procedure a long needle is inserted through the outer abdominal wall and into the gallbladder. A chemical called Methyl tert butyl is then injected to dissolve the stones. The stones usually will dissolve in 1 to 3 days. But this chemical must be used very carefully because it is a flammable anesthetic and is very toxic- you don't want it to enter the bile duct and get into your intestines. The procedure is being tested in patients with symptomatic, noncalcified cholesterol stones. The major drawback (besides the pain of the needle) is that the stones will, unfortunately, come back again. I am not sure how often you can have this done or how often most insurance companies will pay for it.
Stone Fragmentation
Shock-wave lithotripsy is combined with bile acid dissolution in this procedure. You sit in a large tub of water and your gallbladder is bombarded with shockwaves. This does not work very well and you still have to pass the stones out of your bile ducts somehow, or have them surgically removed. Attacks of biliary colic (intense pain) are common after treatment, and ESWL's success rate is not very high. I did not look much into this treatment option since I was told most hospitals do not have the multi-million dollar equipment needed, at least not here where I live. Other nonsurgical methods are still considered experimental, but I just didn't feel like I had the time to experiment with my health!
Wait and See Method
This is where you wait and see if the problems go away. This did not work for me. I changed my diet, got rid of caffeine, did everything I was supposed to, but still had an attack six months later.
Surgery
Surgery to remove the diseased or non-functioning gallbladder is the most common and effective way to treat symptomatic gallstones. (Asymptomatic gallstones usually do not need treatment.) Each year more than 700,000+ Americans have gallbladder surgery successfully. I have not yet read about anyone dying from this procedure. The surgery is called cholecystectomy.
This is what I had done yesterday (October 14, 2005) at Mercy Hospital here in Portland, Maine. I didn’t like the idea of surgery; but after examining every other possible option, talking to various doctors about all the different treatments, reading countless books and articles about the problem and also meeting a lot of people (mostly women) who had this done, and who said it was easy to get through and they bounced right back; I finally decided that the removal of my gallbladder was the best treatment option for me- scary or not. I didn't meet anyone who had had a difficult time with the surgical procedure. Most said it was the best thing they could have done. No regrets.
Here is what happened on my day of surgery:
I arrived at the hospital at 7am where I was checked in and then taken to the "Short Stay Unit" and assigned to room number 6. I changed out of my clothes and into a gown then sat in bed to wait. I was # 2 that day for surgery. I may be a 40-year-old man, but I was happy to have my mother with me! As I waited my mother and I talked about when she had her gallbladder removed in 1972 when she was 28. That was when they had to make the big 8" incision and she said it was a very painful recovery. She said she wished they had this new type of surgery when she had to have it. She also had four children to look after, after her surgery! I remember her surgery. My mother was 28 and had 28 large stones. She had her third and final attack of stones after she ate a donut with some whole milk. She had had enough. We lived in Livermore, CA at the time.
After a while a nurse came in to take my vitals and to show me a device that was going to be placed on my legs during surgery and would still be on for a while afterwards. The machine used air to squeeze and release my legs to help stop any blood clots from forming. That was a good thing, I thought. Then all the hair on my stomach and lower chest was shaved off and the area was scrubbed with a special soap. My mother said she didn't know I had so much hair on my chest...but that it had been a long time since she had changed my diaper! The nurse thought that was very funny. At least I was able to keep my mustache and goatee! Around 8:45 am I told my mother to go and get some errands she needed to do done and that I would be OK- she would be back before I was out of surgery. She hesitantly left and I waited.
At 9:20am the friendly OR prep nurse came into my room and said they were ready for me. Nervously I was wheeled into the OR prep room. There I was asked who I was and what was going to be done today. The staff wants to be 100% sure they have the right person going in for the right treatment. I was then given a painless shot into my left wrist to have my IV line started. Then a solution of electrolytes, plasma and other fluids was sent through my IV, including a light sedative.
Next my anesthesiologist came over to meet with me in the OR prep room and we talked about any concerns I had. He reassured me about the safety of General anesthesia, which was what was going to be used. I had done a lot of research on line and learned that General anesthesia is very safe these days with only 4 or 5 deaths out of every one million persons anesthetized. He checked my chart and said my blood work was very, very good. Some of the best he had seen with a gallbladder patient. After he and I were done talking I was wheeled into the OR which was very bright and very clean and white. I was transferred to the main OR table and draped with warm blankets. My anesthesiologist asked what my body weight was and I told him 155 at just over 6 feet tall. He needed to know the correct weight to use the right amount of anesthesia. After some adjusting of the table I was told they were ready to begin. An oxygen mask was placed over my nose and mouth and I was anesthetized through my IV line. I looked up above me at the operating room lights and started to feel dizzy, then my vision blurred and I was out. I was anesthetized and ready for surgery before my doctor came in. My surgery started promptly at 9:30 am. After my cholecystectomy was completed I had a liver biopsy done since my blood liver tests were high- which can also mean stones are present. I was told this was just a precaution and more than likely nothing to worry about.
I woke up in OR recovery laying on my left side in sort of a fetal position with a nurse asking how I was feeling. I said OK and asked what time it was, it was around 11:30am. My surgery had taken one hour and fifty minutes. After awhile I was then taken back to my room in the short stay unit where my mother was waiting. My doctor had talked to her just before I arrived and told her everything was fine. My liver looked good, but it was irritated by my enlarged and diseased gallbladder. After waking up more, I was dizzy and in very little pain, my throat hurt more than my stomach area, I think mainly due to the tube placed in my throat during the procedure. Gradually the pain in my stomach area got a little worse and I was asked on a scale from one to ten what it was. It hovered at about a four or five, so they offered me some pain medication. I was given two 500mg Vicodin pills to help with pain and it worked very well and very quickly. Also the pain in my right shoulder was irritating, but I was told that it would happen in response to the C02 gas they had used in my abdomen to be able to see clearly during surgery. The pain medication also took the shoulder pain away. I knew I would have some pain after surgery, but that the other horrible problems of having a diseased gallbladder were over after many years of very painful attacks. I was happy about that and could deal with the pain of healing. I suffered no adverse effects from the General anesthesia.
I looked at my abdomen and saw the four small bandages covering my little incisions. I thought about the fact that I no longer had to worry about gallstones and the other possible complications and agonizing pain that came with them and I felt I had done the right thing. I was out of the hospital by 3:15pm when my mother drove me home to rest.
The first night was difficult as far as sleeping went. I could not lie on my right side without a nagging pain. I was afraid to move around too much, though I had been told there was nothing to worry about. I could sleep on my left side, which is how I woke up in recovery, and I could sleep on my back with my knees bent or straight. I slept most of the first day and second day as well due to the Vicodin I was taking. I had filled my prescription for Vicodin on my way home after surgery and it helped a great deal, but I did not need it much past the third day. I do recommend that you sleep in a dim, quiet and cool (comfortable) room with no pets to jump on the bed the first few days. You can be all alone, as I was, as long as you have a phone near your bed in case you need to make a call or for friends and family to call to wish you a speedy recovery.
I will admit (even at 40) I was very scared to have my gallbladder removed, but that is a normal reaction to any surgery for most people. But everything was monitored in the OR and I trusted the hospital staff after voicing my concerns about everything to them.
The following morning I did have some toast and milk and that was met with diarrhea, which I was told may happen. Since that second day things have been mostly normal in terms of my bowels, thankfully. I have not tried a big meal yet, but I will and I will let you know how things are going.
To understand what goes on during this type of surgery please read on:
During laparoscopic cholecystectomy the surgeon makes several tiny incisions in your abdomen and then inserts special surgical instruments and a miniature video camera into your abdomen. The abdomen is also "inflated" with C02 to make it easier for your doctor to see the area clearly. The tiny camera inserted sends a full-color magnified image from inside your body to a video monitor, giving the surgeon a close-up view of the organs and tissues. While watching the monitor, the surgeon uses the instruments to carefully separate the gallbladder from the liver, ducts, and other structures. Then the cystic duct is cut and the gallbladder is removed through one of the small incisions- usually the one just under or in your bellybutton (which does not hurt). The ducts from and the vein supplying blood to the gallbladder are then clipped off and sewn shut.
Because the abdominal muscles are not cut during laparoscopic surgery, patients have less pain and fewer complications than they would have had after surgery using a large "open" incision across the abdomen. Recovery usually involves only one night in the hospital, if that, followed by several days of restricted activity at home. As I said above I was in and out the same day.
If the surgeon discovers any obstacles to the laparoscopic procedure, such as infection or scarring from other operations, the operating team may have to switch to open surgery. In some cases the obstacles are known before surgery, and an open surgery is planned. It is called "open" surgery because the surgeon has to make a 5- to 8-inch incision in the abdomen to remove the gallbladder. This is a major-type surgery and may require about a 2 to 7-day stay in the hospital and several more weeks at home to recover. Open surgery is only required in about 5 percent of gallbladder operations these days.
The most common complication in gallbladder surgery is injury to the bile ducts. An injured common bile duct can leak bile and cause a painful and potentially dangerous infection. Mild injuries can sometimes be treated nonsurgically. Major injury, however, is more serious and requires additional surgery. But most injuries of this type are rare.
If gallstones are in the bile ducts, the physician (usually a gastroenterologist) may use endoscopic retrograde cholangiopancreatography (ERCP) to locate and remove them before or during the gallbladder surgery. In ERCP, the patient swallows an endoscope; a long, flexible, lighted tube connected to a computer and TV monitor. The doctor guides the endoscope through the stomach and into the small intestine. The doctor then injects a special dye that temporarily stains the ducts in the biliary system. Then the affected bile duct is located and an instrument on the endoscope is used to cut the duct. The stone is captured in a tiny basket and removed with the endoscope. I had this done during my surgery to remove a stone from the common bile duct.
Occasionally, a person who has had a cholecystectomy is diagnosed with a gallstone in the bile ducts weeks, months, or even years after the surgery. The two-step ERCP procedure is usually successful in removing the stone.
Complications of gallstones not treated can include:
Cholangitis, Gangrene, Jaundice, Pancreatitis, Sepsis, Fistula, and Ileus. Several of which can lead to death if not treated.
Gallstone Facts and Statistics
Gallstones affect approximately one in ten Americans, and are associated with approximately 3,000 deaths annually.
More than 800,000 hospitalizations each year are caused by gallstones that are large enough to cause significant pain.
Over 700,000+ people undergo surgery for gallstones annually.
Obesity is one of the strongest risk factors for gallstones.
Rapid weight loss diets significantly increase the risk for gallstones.
Wrap-Up:
As I said above I am not a doctor, I simply had gallstones and wanted to let others know about my experience. The thought of surgery was actually far worse than the actual procedure for me. I was scared of being operated on, but I was also scared of having another attack of gallstones. I was also tired of being afraid to eat. I feared food and attacks. I am mostly pain free four days after surgery and getting better each day. My shoulder pain is completely gone and my stomach only hurts when I laugh, cough or slouch while sitting. I now am happy I will never have a gallstone attack again! I welcome your comments and experiences!
Post Note: (October 24, 2005):
I have just returned from my post-op check up. My doctor said my surgery went well (with him I knew it would). My liver biopsy showed fatty material, but looked healthy otherwise and my doctor said I had nothing to worry about. I had 147 stones of various sizes. My bowels are mostly fine with occasional problems-- just like everyone else! Your primary doctor can give you a prescription for Colestipol to control what is usually referred to as "bile acid diarrhea" should it get too bad. Thankfully I have not had to deal with that, but many others have written saying they have and asked what to do about it.. That is about it. I hope this page has helped you to understand your gallbladder and biliary system and let you know some of the options you have to feeling better. After surgery I have to say I am pro-surgery, but before; it was scary. Don't be afraid to be afraid- it's normal! Good luck and Thank You for visiting!
Post Note II: (January 2, 2006):
I wanted to let people know, who have asked, that I am and have been 100% back to normal since late October 2005. I have had no problems at all post-op. The surgery was the best thing I could have done for my health.
Post Note III: (March 8, 2008):
I have been asked many times who I ask when I have questions about Gallbladder problems. I see my physician, Dr. William Dexter at 272 Congress Street here in Portland, Maine and he is wonderful! If you have had surgery and have questions please ask your primary doctor, they want to help you! Also some have asked about nausea. Eat a few Ginger Snaps cookies (not many!) or take some Ginger root caplets with water to treat nausea. It works wonders.
Post Note IV: (January 22, 2012):
Things are still great. I no longer have any issues and have not for many years, I am 100% healthy in all aspects of my life! Many people have written over the years and many people continue to write asking advice, I am very happy to know my page and I have been of some help!! The best thing to remember is to listen to your doctor, they know what is best. If needed get a second opinion. I am enjoying the weather up here in the New England States! I *love* this state! I have not a care in the world... life is beautiful!
"Have no fear, stupid people eventually go away!" ....(my fortune cookie last night! HA HAA!)
Post Note V: (March 30, 2021):
I'm still enjoying my place here in Portland. I live in the upper 170’s on Eastern Promenade in Portland, ME. So many of the houses in this area have been made into apartments. I was very glad to find this house that needed only a bit of work (floor refinishing after carpet removal) in an area that houses are still houses, not apartments! I still love looking out at Portland Harbor and I walk Fort Allen Park and trail every day in spring and summer and into fall! Sometimes I head over to Back Cove. The Back Bay Fireworks are always fun each year. Look for my new blog coming soon directly linked off DanielJSelby.com! I'm going to highlight some good friends here in Portland and some favorite places! I’ve been taking the ferry out to Peaks Island to see friends lately. We gather socially distanced at the Volunteers of America building. More soon!
Post Note VI: (February 2, 2025):
All is well here in Vermont. I left Maine several years ago. I retired from both the nursing field and acting at 58 on 12/31/2023! Also for the last four years I have been researching and compiling discography books for BearManor Media out of Florida. As of January 23, 2025 I have had eight (8) books released. They are available World-Wide in store on-shelf and by special order. You can also find them at BearManor Media's web page and a general search on Google of: Daniel Selby Books will bring them up! Amazon has also placed an Author's Page up for me on their site and all the books are there! Look for my "Book Blog" linked off the main page coming in the near future!
Later!
~Daniel Selby
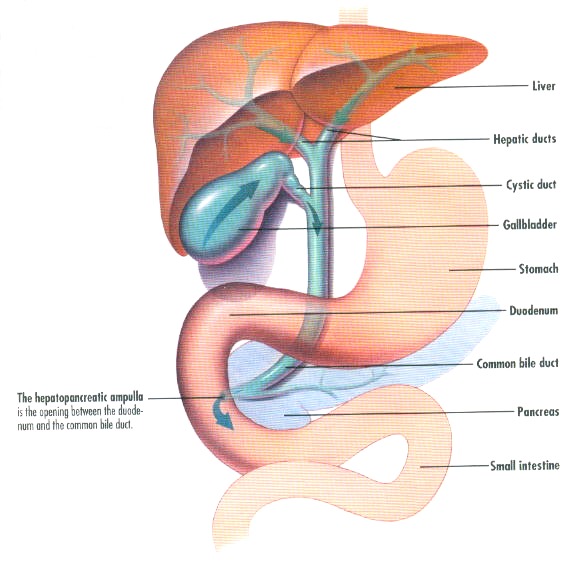
The Gallbladder/Biliary System
E-mail Me!
If you do write (and I would love to hear from you) please put "Gallbladder" in the subject line so I do not think the email is spam and delete it. Thanks!
Page created on October 15, 2005. Finished October 17 & 18, 2005.
Page Updated February 2, 2025
©2005-2025 Daniel Selby / 80 Powers
(**My 20th Year!**)
